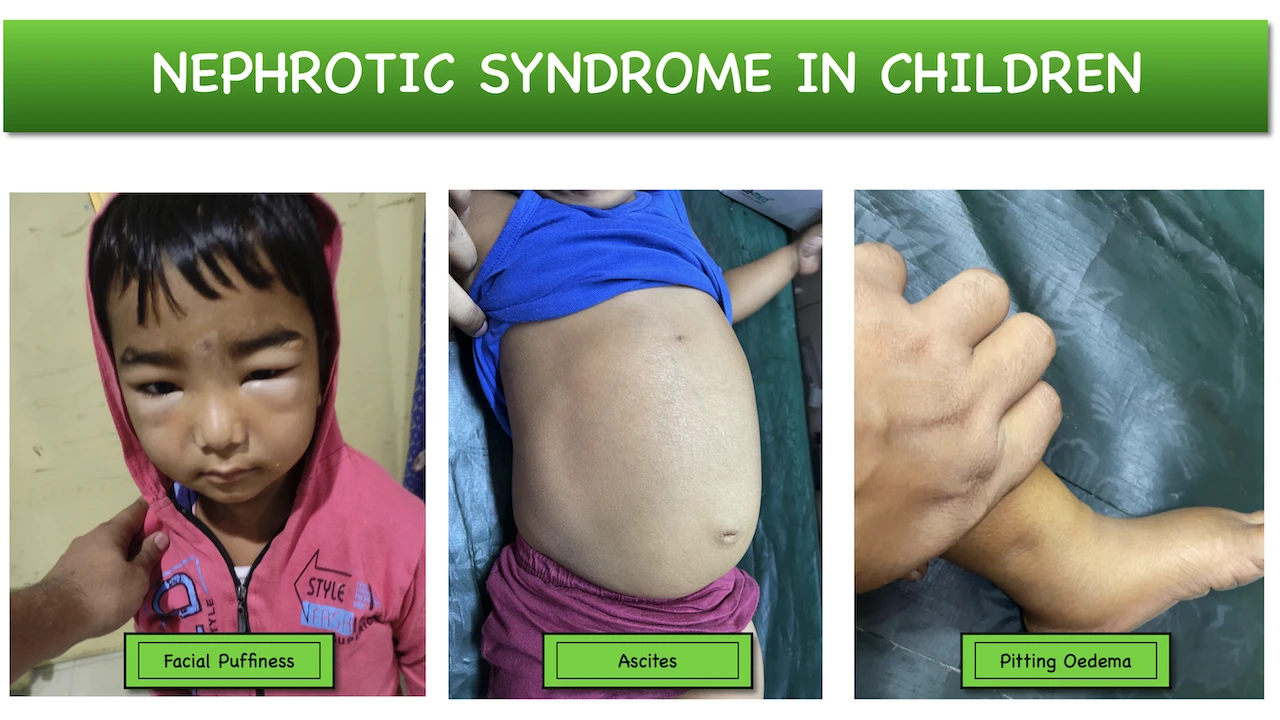
Nephrotic syndrome is a disorder of kidney in which so many abnormalities can be found in the kidney due to some pathology. The child can present with massive proteinuria, generalised oedema, hypoalbuminemia and hyperlipidemia.
1. Causes :
In case of children there are mainly two types of causes, one is Primary causes and another one is secondary causes.
I. Primary causes :
They are :
- Congenital nephrotic syndrome
- Membranous nephropathy
- Focal segmental sclerosis
- Diffuse mesangial sclerosis
- Minimal change disease
II. Secondary causes :
They are :
- Infections : Syphilis, HIV, Malaria Cytomegalovirus, Toxoplasmosis, Rubella, Hepatitis B.
- Syndromes with associated renal disease : Lowe syndrome, Nail-patella syndrome, Denys-rash syndrome, Nephropathy associated with congenital brain malformation.
- Systemic lupus erythematosus
- Haemolytic ureic syndrome
- Drug reactions : Toxins and Mercury
2. Clinical Faetures :
- Edema : The onset of oedema is insidious in nature, and first appear surrounding the eye, then slowly progress to become generalised and forms ascites, hydrothorax and hydrocele.
- Ascites
- Pitting Oedema
- If infection is the cause then slight rise of temperature can be noticed.
- Severe muscle wasting can be see.
3. Pathophysiology :

A. Massive proteinuria and Hypoalbuminemia :
Any structural or physiochemical change can affect the GBM(Glomerular basement membrane), which may lead to increase the permeability to plasma protein. Which will enhance protein excretion and cause Massive proteinuria. As a result serum albumin will decrease and will cause Hypoalbuminemia. As a result of decrease in Serum albumin, drop in plasma oncotic pressure will occur.
B. Generalised edema :
- Now the decreased intravascular volume and renal blood flow will cause secretion of renin from renal juxtaglomerular cells.
- Then renin further stimulates angiotensin-aldosterone axis, this will promote the water and salt retention by kidney.
- Now this water and salt retention along with hypoalbuminemia will cause localised oedema at first, and further this will form generalised oedema,
C. Hypolipidemia and Lipiduria :
- Here, Hypoalbuminemia triggers the synthesis of lipoproteins in the liver, or sometimes massive proteinuria causes loss of an inhibitor of their synthesis.
- This will cause Hyperlipidemia and lipiduria.
4. Management :
A. Investigations :
- Urine examination : Heavy proteinuria – 3+ to 4+, Hyaline and granular should be present.
- Serum albumin : This will be low and value will remain < 1g/dL.
- Hypercholesterolemia : This may show milky appearance to the plasma.
- Blood urea and creatinine : Remains in normal range.
- Antibody titre : IgG will decrease but IgM will be elevated.
B. Treatment :

There are mainly two types of treatment done in Nephrotic syndrome, one is Supportive treatment and another one is Specific treatment.
I. Supportive treatment :
- Low salt diet intake.
- Using Diuretics to excrete extracellular water and reduce oedema. Diuretics used are : Frusemide, Hydrochlorthiazide or Metolazone, and Spironolactone.
- ACE Inhibitors : Enalapril or Ramipril is used.
- 20% salt free albumin at the end of albumin infusion if serum albumin is <1gm/dL with hypovolemia.
II. Specific treatment :
In specific treatment, there are 4 various types of treatment based on different scenario. The different scenarios can be :
- We can start the Initial therapy.
- Infrequent & Frequent Relapse of Nephrotic syndrome.
- Steroid dependent Nephrotic syndrome.
- Steroid Resistant Nephrotic syndrome.
A. Initial therapy :
In initial therapy the drug used is Prednisolone. At first it is started with 2mg/kg/day, divided into twice or thrice doses for 6 days. Then 1.5 mg/kg on alternate day at single morning dose for 6 days. Most patient gives response by the end of 2nd week of Prednisolone therapy, those are called Early responder. Few patient responds after 4-5 weeks of Prednisolone, those are called Late responder. If not responded till 8th week of Prednisolone then those are known as Steroid resistant Nephrotic syndrome.
B. Treatment in Infrequent & frequent relapse :
Relapse in Nephrotic syndrome signifies : Edema/First morning urine sample contains 3+ or 4+ protein for consecutive 3 days.
- Infrequent relapse means <=3 relapses in a year & Frequent relapse means >=4 relapses in a year.
- Treatment of Infrequent relapse in Nephrotic syndrome : Prednisolone 2mg/kg/day, divided into twice or thrice doses until urine protein negative or trace for 3 consecutive days. Then 1.5 mg/kg on alternate day single morning doses for 4 weeks.
- Treatment of Frequent relapse : This treatment is same as Steroid dependent Nephrotic syndrome, discussed in below section.
C. Steroid dependent Nephrotic Syndrome and Treatment :
This is known as occurrence of two consecutive relapses during alternate day Prednisolone or within 14 days of stopping Prednisolone.
- Initially Prednisolone is used 0.25-0.7 mg/kg for alternate day in single dose up to 9-12 months. Or, Levamisole 2-2.5 mg/kg on alternate day for 1-2 years. Adding Initially continuing alternate day single dose Prednisolone 0.75-1 mg/kg for few weeks then gradually taper and stopped.
- Cyclophosphamide : 2-2.5 mg/kg/day for 12 weeks in addition with Alternate day single dose prednisolone 1-1.5 mg/kg for 12 weeks.
- Cyclosporine : 4-5 mg/kg/day in two divided doses for 1 year, in addition with Alternate day Prednisolone for 12 weeks.
- Mycophenolate Mofetil : 20-25 mg/kg/day in two divided doses for 1-2 years with tapering dose of prednisolone.
- Tacrolimus : 0.15 mg/kg/day in two divided doses for 2 years, in addition with Alternate day Prednisolone.
- Rituximab : This is a monoclonal anti-CD20 antibody. This is useful in patients who shows toxicity to other drugs.
D. Steroid resistance Nephrotic syndrome(SRNS) and Treatment :
- Cyclophosphamide : 2-2.5 mg/kg/day oral for 12 weeks, in addition with Alternate day single dose of Prednisolone 1-1.5 mg/kg for 12 weeks.
- Pulse Therapy : Inj. Methylprednisolone 30mg/kg on alternate day, total doses 3-6. In Refractory SRNS, The dose is continued once in a week for next 8 weeks, then twice a month for next 2 months, and then once in a month for next 6-12 months. Followed by alternate day single dose prednisolone starts at 1.5mg/kg then tapering up to 0.25 mg/kg for 4-12 months.
- Inj. Cyclophosphamide : It is given with dose of 500mg/m2 IV for 6 months.
- Cyclosporine : 4-5 mg/kg/day in two divided doses for 1 year, in addition with alternate day Prednisolone for 12 weeks.
- Tacrolimus : 0.15 mg/kg/day in two divided doses for 2 years, in addition with alternate day Prednisolone.
- Rituximab : It is given with dose of 375 mg/m2/week for 4 weeks.